Thalassaemia is the most common inherited blood disorder in Malaysia, yet many remain unaware that they may be silent carriers of this lifelong condition [1, 2]. Passed down silently through generations, this disease impairs the body’s ability to produce healthy haemoglobin (the oxygen-carrying protein in red blood cells), leading to chronic anaemia, severe physical complications, and a significantly reduced quality of life if left unmanaged [3].
Malaysia is considered a thalassaemia hotspot, particularly among the Malay, Chinese, and indigenous ethnic groups. Between 4.5% and 6.8% of Malaysians are thalassaemia carriers [4, 2], and cases are rising despite existing public health efforts. With early detection, timely treatment, and preventive health screenings, many complications can be avoided—making awareness a public health imperative.
What Is Thalassaemia and How Does It Affect the Body?
Thalassaemia is a genetic blood disorder that results from mutations affecting the production of alpha or beta globin chains in haemoglobin [3]. Without enough functioning haemoglobin, the body can’t get the oxygen it needs, leading to low haemoglobin, low red blood cells, and chronic anaemia [3].
There are two main types of thalassaemia:
- Alpha thalassaemia happens when one or more of the four alpha-globin genes is missing. Most people with one or two missing genes have no symptoms or only mild anaemia, but in rare cases where all four are absent, the result is fatal even before birth [3].
- Beta thalassaemia results from mutations in the beta-globin gene. If both copies are defective, the child may develop beta thalassaemia major, which presents early in life (between 6 to 24 months of age) and requires lifelong transfusions [5]. Beta thalassaemia intermedia is a milder form that still causes anaemia and complications, while beta thalassaemia minor (carrier state) is usually asymptomatic [6].
Common symptoms include [3]:
- Persistent fatigue and weakness
- Pallor or yellowish skin
- Dizziness and fainting
- Slow growth in children
- Shortness of breath
In severe cases, patients may develop [1,7, 8]:
- Enlarged spleen or liver (hepatosplenomegaly)
- Bone deformities (thalassaemia facies)
- Iron overload from repeated transfusions
- Delayed puberty and infertility
- Hepatitis B and C infections due to transfusion risks
- Cardiac failure, arrhythmias, and liver cirrhosis due to iron overload
Carriers often show no symptoms, underscoring the importance of thalassaemia screening in Malaysia.
Thalassaemia in Malaysia: A Widespread and Growing Concern
Malaysia’s high carrier rate—between 4.5% to 6.8% of the population—makes thalassaemia the country’s most common genetic disorder [4, 2]. The latest Malaysian Thalassaemia Registry reported 7,984 patients as of 2018, with 34.37% diagnosed with haemoglobin E/β-thalassaemia, the most prevalent subtype [2].
Ethnic distribution reveals that Malays make up nearly 64% of thalassaemia cases in Malaysia, followed by Chinese (12%) and Kadazan-Dusuns (11%) [1]. Sabah accounts for the highest number of cases by state (22.72%) [2].
Alarmingly, many carriers remain undiagnosed due to the asymptomatic nature of the condition. When two carriers have children, the risk of giving birth to a child with thalassaemia major is 25% with each pregnancy [3].
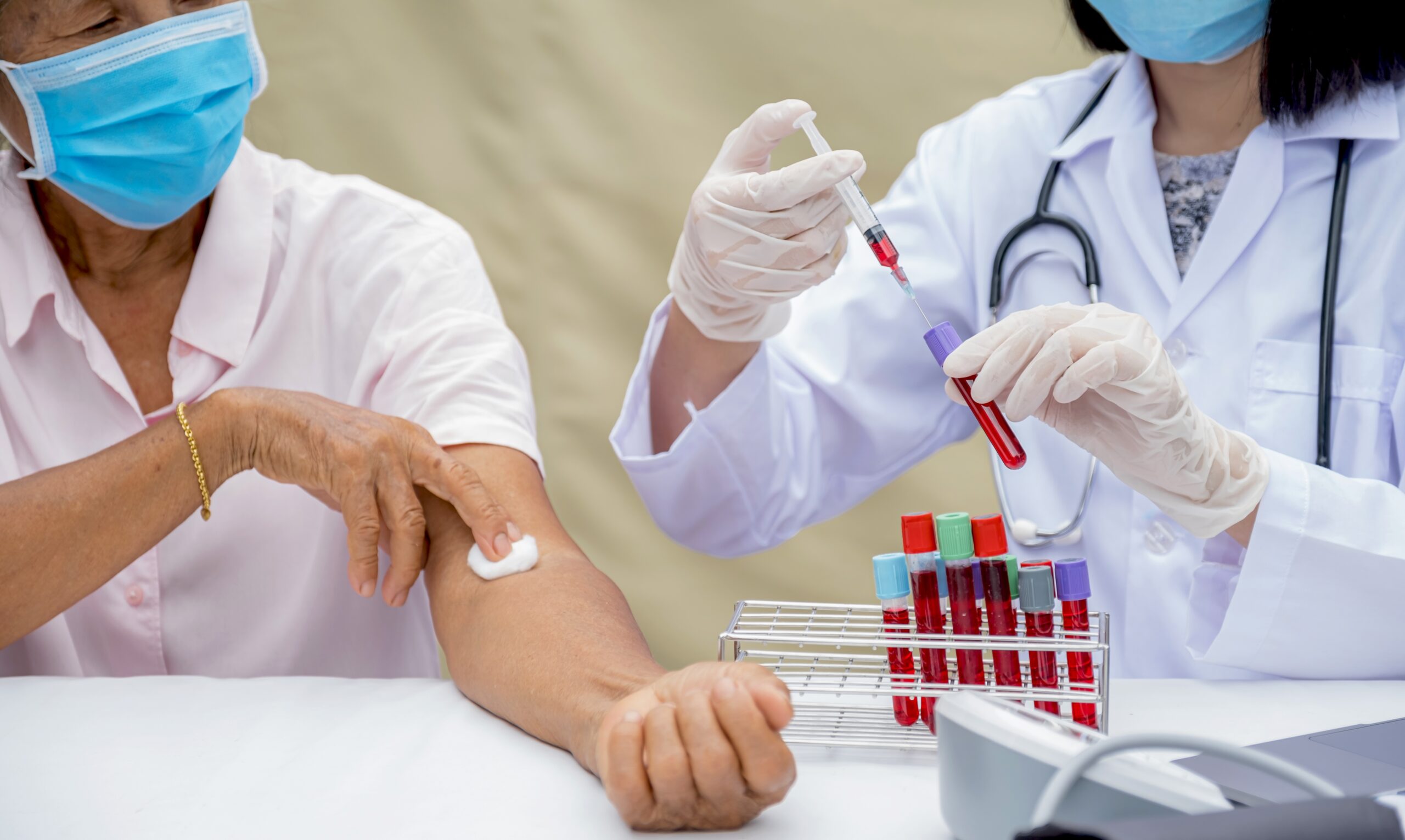
How Is Thalassaemia Diagnosed in Malaysia?
Diagnosing thalassaemia starts with a Full Blood Count (FBC), where key red cell indices—like MCV (Mean Corpuscular Volume) and MCH (Mean Corpuscular Haemoglobin)—may show smaller, paler-than-normal red blood cells [7]. According to Malaysia’s Ministry of Health, individuals with MCH < 27 pg should be screened for thalassaemia [7].
This is followed by [7]:
- Haemoglobin electrophoresis to detect abnormal haemoglobin types
- Genetic testing to confirm carrier or patient status
- Cascade screening for immediate and extended family members if a carrier or patient is identified
Treatment Options for Thalassaemia in Malaysia
There’s no “one size fits all” approach. Treatment depends on the type and severity—but for those with transfusion-dependent thalassaemia (TDT), it’s a lifelong balancing act between managing anaemia and preventing iron overload [7].
1. Blood Transfusions
Regular packed red blood cell (PRBC) transfusions are essential for survival in thalassaemia major. However, repeated transfusions lead to iron overload, which can damage the heart, liver, and endocrine organs [7].
2. Iron Chelation Therapy
To remove excess iron, patients are prescribed iron chelation therapy using medications like [7]:
- Desferrioxamine (infusion)
- Deferasirox (oral)
- Deferiprone (oral)
Consistent chelation is critical to survival. Without it, cardiac failure becomes the leading cause of death in TDT patients, accounting for up to 71% of deaths [2, 5].
3. Splenectomy
In some cases, splenectomy is required to reduce transfusion needs. However, the risk of overwhelming post-splenectomy infection (OPSI) is high, especially in young children, with a mortality rate of up to 69% [5].
4. Bone Marrow Transplant
The only curative treatment for thalassaemia is a haematopoietic stem cell transplant from a matched donor. Unfortunately, this option is not always available or feasible, especially in low-resource settings [7].
Why Thalassaemia Screening in Malaysia Is Crucial
Identifying carriers before pregnancy is crucial in reducing the birth of children with transfusion-dependent thalassaemia (TDT). While there is no universal cure, early detection can lead to better management, reduced complications, and more informed reproductive decisions through thalassaemia and genetic counselling [7].
Malaysia has made notable strides in thalassaemia screening. Since 2016, school-based screening has been implemented for Form 4 students. Students give a small blood sample, receive their results, and are offered counselling if identified as carriers. A thalassaemia screening card is also provided for future family planning [9].
This proactive approach is crucial—thalassaemia carriers show no symptoms but can pass on the condition if both partners are carriers. According to Rahim et al. (2024), countries that implemented comprehensive screening and counselling programmes saw a marked reduction in thalassaemia births [10]. More importantly, the cost of screening is 23–65 times less than the lifetime treatment cost of a single patient [10].
In Malaysia, premarital and antenatal thalassaemia screening is also offered, with counselling options provided through public health clinics [7].
Screening is particularly important for individuals with chronic anaemia, a family history of blood disorders, or those of Malay, Chinese, or indigenous descent—who statistically have higher carrier rates, as well as couples planning a pregnancy or marriage [4, 1].
Living with Thalassaemia in Malaysia: Challenges Beyond the Clinic
The physical and emotional toll on thalassaemia patients and their families is immense. A study by Foong et al. (2022) found that [1]:
- 45% of patients have comorbidities, and 9% have multiple complications
- Many experience poor physical and mental health several days a month
- 36% were unemployed, while 38% earned under RM1,000 monthly
- Patients expressed frustration with healthcare systems and societal stigma
For many, managing thalassaemia means balancing health with work, family, and financial obligations. One respondent described it as “facing more life disruption in a rather non-supportive community” [1].
The financial cost of managing thalassaemia is equally heavy—averaging USD 606,665 per patient, with most of it spent on iron chelation therapy [11]. Countries like Singapore and Cyprus have shown that investing in screening programmes is more cost-effective in the long run [10].
Where to Get a Thalassaemia Test in Malaysia
Thalassaemia screening is available at selected Qualitas Health Malaysia clinics as part of routine blood health check-ups and genetic disease screening services.
We offer:
- Affordable thalassaemia blood test packages
- Full Blood Count test and genetic screening services
- Genetic counselling and family cascade testing
- Comfortable and confidential screening environments
Visit our clinics page to find a Qualitas Health clinic near you.

Blood Donation: A Lifeline for Thalassaemia Patients
Patients with transfusion-dependent thalassaemia (TDT) require regular transfusions to survive. You can support them by being a blood donor.
One pint of blood could mean everything to someone living with thalassaemia. Let your contribution be part of the solution.
Conclusion
Thalassaemia in Malaysia is not just a medical issue—it’s a public health challenge with wide-reaching consequences for individuals, families, and the healthcare system. While treatment exists, prevention through early screening and education is the most effective and sustainable path forward.
Whether you’re feeling tired for unknown reasons, have a family history of anaemia, or are planning to start a family, a simple thalassaemia test could change everything.
FAQs
- What causes thalassaemia?
Thalassaemia is a genetic disorder passed down from parents. It affects haemoglobin production and results in anaemia. - What are the early signs?
Fatigue, paleness, shortness of breath, jaundice, and growth delays. Carriers often have no symptoms. - Can thalassaemia be cured?
While there is no universal cure, treatments like regular blood transfusions, iron chelation therapy, and bone marrow transplants (in select cases) can help manage the condition. - Is thalassaemia screening safe and accurate?
Yes. Standard thalassaemia tests in Malaysia involve routine blood draws and are safe, accurate, and non-invasive. Fasting is not required. - How much does thalassaemia screening cost in Malaysia?
Costs vary, but Qualitas Health Malaysia offers affordable thalassaemia screening. Contact your nearest clinic for details. - Who should get screened?
Anyone planning to have children, especially if from high-risk ethnic groups or with family history.
References
[1] Foong, W. C., Chean, K. Y., Rahim, F. F., Goh, A. S., Yeoh, S. L., & Yeoh, A. A. C. (2022). Quality of life and challenges experienced by the surviving adults with transfusion dependent thalassaemia in Malaysia: a cross sectional study. Health and Quality of Life Outcomes, 20(1). https://doi.org/10.1186/s12955-021-01897-4
[2] Ibrahim, H. M., Muda, Z., Othman, I. S., Mohamed Unni, M. N., Teh, K. H., Thevarajah, A., Gunasagaran, K., Ong, G. B., Yeoh, S. L., Muhammad Rivai, A., Che Mohd Razali, C. H., Din, N. D., Abdul Latiff, Z., Jamal, R., Mohamad, N., Mohd Ariffin, H., & Alias, H. (2020). Observational study on the current status of thalassaemia in Malaysia: a report from the Malaysian Thalassaemia Registry. BMJ Open, 10(6). https://doi.org/10.1136/bmjopen-2020-037974
[3] Thalassaemia . (2022, June 1). National Heart, Lung, and Blood Institute. https://www.nhlbi.nih.gov/health/thalassaemia/causes
[4] Alwi, Z. B., & Syed-Hassan, S.-N. R.-K. (2022). Thalassaemia in Malaysia. Hemoglobin, 46(1), 45–52. https://doi.org/10.1080/03630269.2022.2057326
[5] Management of Transfusion Dependent Thalaessemia. (2009). Ministry of Health Malaysia. https://mpaeds.my/wp-content/uploads/2018/03/CPG-Management-of-Transfusion-Dependent-Thalassaemia.pdf
[6] Yusof, W., Zulkifli, M. M., Azman, N. F., Ab Hamid, S. A., Othman, A., Draman, N., Zilfalil, B. A., Hassan, R., & Abdullah, W. Z. (2020). Factors affecting health-related quality of life and its association with the Xmn1-Gγ polymorphism among adolescents with transfusion-dependent beta thalassaemia and HbE/Beta thalassaemia in East Coast Malaysia. Pediatric Hematology Oncology Journal, 5(2). https://doi.org/10.1016/j.phoj.2020.04.001
[7] Clinical Practice Guidelines: Management of Thalassaemia. (2024). In Portal Rasmi Kementerian Kesihatan Malaysia. Malaysian Health Technology Assessment Section . https://www.moh.gov.my/moh/resources/Penerbitan/CPG/Haematology/e-CPG_Management_of_Thalassaemia_(Second_Edition).pdf
[8] Thalassaemia . (2022, October). NHS. https://www.nhs.uk/conditions/thalassaemia/living-with/
[9] Health Inspection at School. (n.d.). MyGovernment ; National Digital Department. https://www.malaysia.gov.my/portal/content/30263
[10] Rahim, A. S. A., Rahim, N. E. H. A., & Jaafar, S. (2024). A systematic review on thalassaemia screening and birth reduction initiatives: cost to success. Medical Journal of Malaysia, 79(3). https://www.e-mjm.org/2024/v79n3/thalassaemia-screening.pdf
[11] Shafie, A. A., Wong, J. H. Y., Ibrahim, H. M., Mohammed, N. S., & Chhabra, I. K. (2021). Economic burden in the management of transfusion-dependent thalassaemia patients in Malaysia from a societal perspective. Orphanet Journal of Rare Diseases, 16(1). https://doi.org/10.1186/s13023-021-01791-8

